When your prescription costs more than your groceries, you’re not alone. Around 29% of Americans say they struggle to afford their medications. For many, this isn’t just inconvenient-it’s dangerous. Skipping doses, cutting pills in half, or not filling prescriptions at all leads to worse health outcomes, more ER visits, and higher long-term costs. But there’s a proven, safe, and often overlooked way to cut your medication bill without sacrificing effectiveness: asking for a therapeutic alternative.
What Is a Therapeutic Alternative?
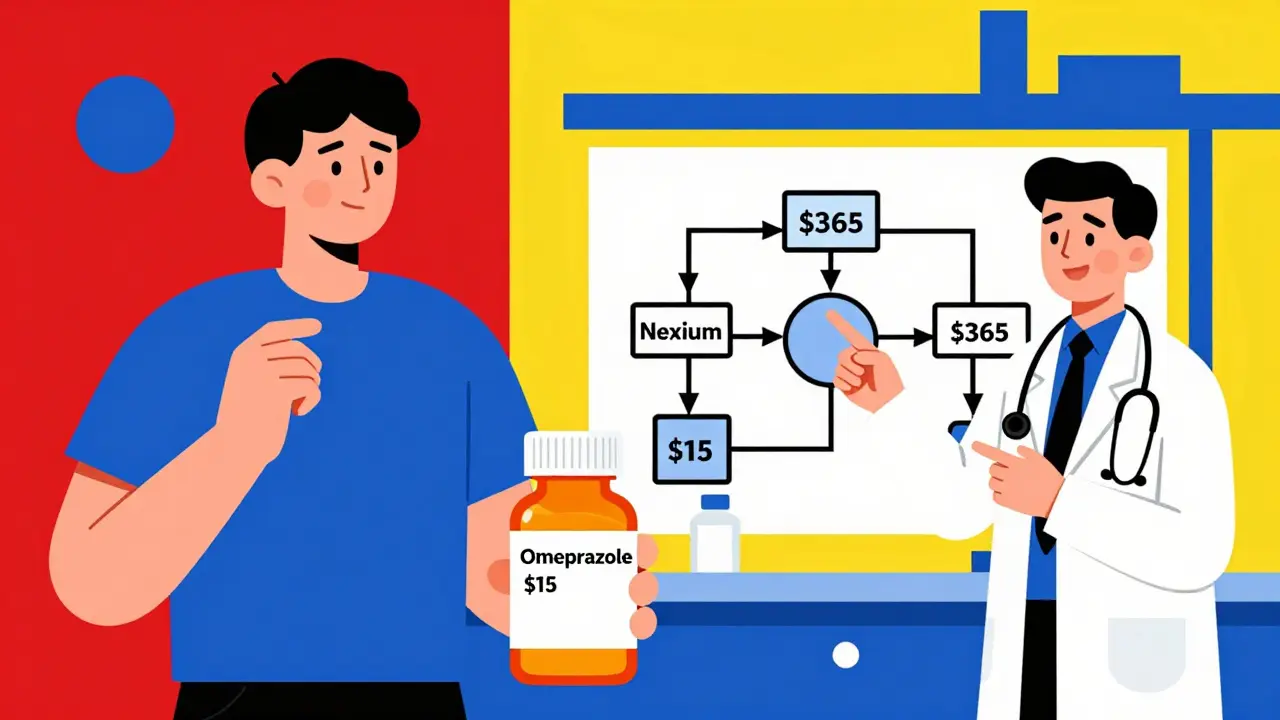
A therapeutic alternative isn’t a generic version of your drug. It’s a different medication that works the same way in your body. For example, if you’re taking esomeprazole (Nexium) for heartburn, your doctor might suggest switching to omeprazole. Both are proton pump inhibitors. Both reduce stomach acid. But omeprazole costs about $15 a month instead of $365. That’s a 96% drop. This isn’t guesswork. Therapeutic interchange-the formal process of swapping one drug for another with similar effects-is backed by clinical studies. A 2017 Vanderbilt study found that when doctors used decision tools to suggest alternatives, patients saved an average of $17.77 per month with no drop in effectiveness. The American College of Physicians, the American Academy of Family Physicians, and even Medicare now support this approach. The key difference? Generic substitution replaces your drug with the exact same chemical, just cheaper. Therapeutic interchange swaps it for a different chemical that does the same job. This matters because sometimes, there’s no generic available-like with newer drugs for diabetes or high blood pressure. That’s where therapeutic alternatives step in.When It Works Best
Not every medication has a good alternative. But for many common conditions, the options are strong:- Blood pressure: Switching from brand-name amlodipine to generic lisinopril can save $300+ a year.
- Diabetes: Jardiance (empagliflozin) costs $600/month. Generic metformin? $10. Many patients do just as well.
- Cholesterol: Crestor (rosuvastatin) vs. generic atorvastatin-same effect, 80% cheaper.
- Depression: Lexapro (escitalopram) can often be swapped for generic citalopram with similar results.
- Acid reflux: Omeprazole instead of esomeprazole saves hundreds monthly.
How to Ask for One
Asking for a therapeutic alternative sounds intimidating. But it’s simpler than you think. Here’s how:- Start with the cost question. Before your next appointment, ask yourself: "Do I ever skip doses because of cost?" If yes, you’re a candidate.
- Bring your pill bottle or list. Write down every medication you take, including over-the-counter ones. Include the dose and how often you take it.
- Ask directly. Say: "I’m having trouble affording this medication. Is there another drug in the same class that works just as well but costs less?" Be specific. For example: "Could I try generic omeprazole instead of esomeprazole?"
- Ask about extended prescriptions. A 90-day supply often costs less than three 30-day ones. Many insurers charge the same copay regardless of supply length. Ask: "Can I get a 90-day supply to save money?"
- Check GoodRx. Go to GoodRx.com or use the app. Enter your drug. See how prices vary between pharmacies. Sometimes, the cash price at Walmart is lower than your insurance copay.
- Ask about patient assistance programs. Most drug makers offer coupons or free programs if you’re under a certain income. Websites like NeedyMeds and RxAssist list them for free.
What Your Doctor Needs to Know
Doctors aren’t always trained to think about cost. Many assume brand names are better. But research shows otherwise. A 2023 AAFP survey found that 37% of patients were initially turned down when asking for alternatives. To help your doctor say yes:- Bring printouts from GoodRx showing price comparisons.
- Share data from studies. For example: "A 2017 study in JAMA found no difference in outcomes between patients on brand-name and generic statins."
- Point out that therapeutic interchange is endorsed by the American College of Physicians and the CDC.
- Ask if your doctor has access to clinical decision tools. Many EHR systems now flag cheaper alternatives at the point of prescribing.

Why Some Doctors Resist
Not every switch works. Some medications have subtle differences. For example, two GLP-1 drugs for diabetes might lower blood sugar equally, but one might cause more nausea. Or one might be better for someone with kidney disease. A 2021 study in JAMA found that 8-12% of patients had different results when switching between similar drugs. That’s why doctors need to be cautious. But that doesn’t mean they should say no. The best approach? Trial and monitor. Ask: "Can we try the cheaper option for 6 weeks? If my symptoms come back, we’ll switch back." Most doctors will agree if you’re willing to monitor your health.What to Do If You’re Refused
If your doctor says no, don’t give up. Ask why. If it’s because they’re unfamiliar with alternatives, offer to help. Say: "Can we look up the guidelines together? I found a study that shows these two drugs are equally effective." If they still refuse:- Request a tiering exception through your insurance. Many plans allow exceptions if a drug is too expensive. You’ll need a letter from your doctor saying the current drug is medically necessary.
- Call your pharmacy. Sometimes, pharmacists can suggest alternatives or help you apply for manufacturer coupons.
- Use the HealthWell Foundation or Patient Advocate Foundation. Both offer financial help for therapeutic switches.
Real Stories
One patient in Sydney switched from Lyrica (pregabalin) to generic gabapentin. Her monthly cost dropped from $450 to $15. Her neurologist was hesitant at first-but agreed after she showed data on effectiveness for nerve pain. Another switched from Eliquis to warfarin. Her out-of-pocket cost went from $450 to $8 a month. She’d been skipping doses because she couldn’t afford it. After the switch, she took every pill. Her stroke risk dropped. But not all stories are smooth. One patient switched from Jardiance to metformin and ended up with uncontrolled blood sugar. She had to go back. That’s why monitoring matters. Always check in with your doctor after a switch.
Tools to Use
- GoodRx: Compares prices across 70,000+ U.S. pharmacies. Works even if you have insurance.
- NeedyMeds: Lists patient assistance programs for over 1,200 medications.
- RxAssist: Free directory of drug discount programs, including state and federal aid.
- HealthWell Foundation: Offers up to $387/month in copay help for 1,200+ medications.
- Medicare Part D: If you’re on Medicare, you can request a tiering exception. By law, it must be processed within 72 hours for urgent cases.
What’s Changing in 2026
New tools are making therapeutic interchange easier. In late 2024, Epic and Cerner-two major electronic health record systems-rolled out upgrades that automatically suggest cheaper alternatives when a doctor writes a prescription. One hospital system saw a 15% jump in switches after the update. The Inflation Reduction Act is also helping. Medicare is now negotiating prices for 10 high-cost drugs. While this won’t fix everything, it means fewer people will need to switch. But experts warn: even with price negotiations, therapeutic interchange will still save money. Oliver Wyman’s 2025 report says negotiated prices are still 20-40% higher than therapeutic alternatives.Final Thoughts
You don’t have to choose between your health and your wallet. Therapeutic alternatives aren’t a last resort-they’re a smart first step. They’re backed by science, endorsed by doctors, and used by millions. Start by asking one question: "Is there a cheaper drug that works the same?" Bring your pill bottle. Use GoodRx. Be ready to monitor your symptoms. Most doctors will say yes if you’re informed and respectful. Saving money on medication isn’t about cutting corners. It’s about working smarter. And with the right approach, you can stay healthy-and keep more money in your pocket.Can I ask for a therapeutic alternative even if I have insurance?
Yes, absolutely. Insurance doesn’t always cover the cheapest option. Sometimes, your copay is higher than the cash price at a pharmacy like Walmart or CVS. Even with insurance, you can ask your doctor if a different drug in the same class might cost less. Many insurers encourage therapeutic interchange because it reduces overall spending.
Are therapeutic alternatives as safe as my current medication?
In most cases, yes. Therapeutic alternatives are chosen based on clinical studies that show they work similarly in terms of effectiveness and safety. For example, multiple studies have shown that generic lisinopril and brand-name benazepril work just as well for high blood pressure. However, some patients may respond differently due to individual biology. That’s why doctors recommend starting with a short trial period and monitoring your symptoms.
What if my doctor says there’s no cheaper alternative?
Ask for specifics. Some drugs truly have no good alternatives, especially in oncology or rare conditions. But for common conditions like diabetes, hypertension, or acid reflux, alternatives usually exist. Ask your doctor to check resources like GoodRx or the $4 generic list at major pharmacies. If you’re still unsure, ask for a referral to a pharmacist who specializes in medication therapy management-they can review all your drugs for cost-saving opportunities.
Can I switch to a therapeutic alternative on my own?
No. Never stop or switch medications without talking to your doctor first. Even if a drug seems similar, changing without medical supervision can be dangerous. For example, switching from one blood thinner to another without proper monitoring can increase your risk of stroke or bleeding. Always get approval from your provider before making any change.
How long does it take to get a therapeutic alternative approved?
If your doctor prescribes it directly, you can get it the same day. If your insurance requires prior authorization, it usually takes 1-3 business days. For urgent cases, Medicare and many private plans must approve exceptions within 72 hours. If you’re waiting longer than a week, call your insurer and ask for an appeal.
Do therapeutic alternatives work for everyone?
Most people do well, but not everyone. Some individuals metabolize drugs differently, or have allergies or other conditions that make one drug better than another. For example, someone with kidney disease might need a different type of diabetes medication than someone without. That’s why doctors consider your full health history before switching. If you notice new side effects or worsening symptoms after a switch, contact your doctor right away.
Are there any medications where therapeutic interchange doesn’t work?
Yes. About 15% of specialty medications-especially biologics used for cancer, autoimmune diseases, or rare conditions-have no therapeutic alternatives. These drugs are complex and often made from living cells, so they can’t be easily swapped. But for the majority of prescriptions (over 80%), alternatives exist. If you’re on one of these rare drugs, focus on patient assistance programs or manufacturer coupons instead.




Christina VanOsdol
February 25, 2026 AT 12:11Alfred Noble
February 25, 2026 AT 14:02Brooke Exley
February 25, 2026 AT 18:55Gabrielle Conroy
February 26, 2026 AT 21:44Natanya Green
February 27, 2026 AT 22:10Emily Wolff
February 28, 2026 AT 17:22Joseph Cantu
March 1, 2026 AT 20:53Khaya Street
March 2, 2026 AT 08:04John Smith
March 3, 2026 AT 08:34Matthew Brooker
March 4, 2026 AT 04:00Nick Hamby
March 4, 2026 AT 17:06kirti juneja
March 6, 2026 AT 11:08Haley Gumm
March 7, 2026 AT 00:38Jacob Carthy
March 8, 2026 AT 05:34Nick Hamby
March 9, 2026 AT 18:42